|
A recent bronchiectasis conference revealed a surprising statistic: only 50% of the audience expressed willingness to participate in clinical trials!!!
While some may be hesitant to take medications without more detailed information, there are other ways to contribute to research. Options for Participation: *Surveys and interviews: Participating in surveys helps researchers better understand patient needs and satisfy FDA requirements for patient participation. Many trials cannot move forward without completed surveys from us. *Patient Advocacy Groups: Registries like EMBARC and the COPD Foundation’s Bronchiectasis Research Registry gather valuable data and researchers use it for their studies. *Biobanks: My experience at NYU Langone highlights the diverse nature of research participation. I agreed to participate in Dr. Leo Segal’s biobank (sputum, blood, potentially stool) to understand how factors like bacteria, viruses, fungi and gut health influence disease progression. This research could pave the way for personalized treatments based on individual microbiomes. Let’s educate ourselves about research opportunities and become active participants. Together, we can make progress in developing new treatments for bronchiectasis. Had the researchers asked the audience what percentage of people would like new treatments, I bet the answer would’ve been 100%. To make new treatments a reality we need to step up!!!✨✨✨ #StepUp #NewTreatments #ClinicalTrials #ClinicalTrialSurveys #ClinicalTrialInterviews #MakeADifference #MakeADifferenceToday #Bronchiectasis #a1at #PrimaryCiliaryDyskinesia #phagetherapy #maclung #maclungdisease
0 Comments
Many in our bronchiectasis and NTM lung disease communities face daily challenges. But there’s also reason for hope! Exciting new treatments are in development.
While we wait for these advancements, let’s focus on what we can control: optimizing our well-being. This includes: 🌟Nutrition: Prioritize nutrient-rich foods to fuel your body’s natural defenses. 🌟Weight Management: Maintaining a healthy weight can improve lung function. 🌟Exercise: Regular physical activity enhances overall health and lung capacity. 🌟Airway Clearance Techniques: Manage mucus build-up to keep airways clear. 🌟Stress Management: Find healthy ways to manage stress, which can worsen symptoms. 🌟Rest and Sleep: Prioritize quality sleep for optimal healing and immune function. Remember, even the most effective treatments work best with a strong foundation of self-care. Let’s empower ourselves by taking charge of our health, one step at a time. I’ll continue sharing valuable no-cost information through social media, YouTube, my website, my website blog and newsletter. I also offer individual consultations and have a book available on Amazon, “The BE CLEAR Method to Living with Bronchiectasis.” As highlighted at recent conferences like ELF/EMBARC and NYU Langone, innovative treatments are on the horizon. We have repurposed drugs, new medications, inhaled therapies, and even bacteriophages (viruses that target specific bacteria) under investigation. Let’s commit to supporting one another on this journey. Progress, not perfection, is key. Celebrate small victories and remember, you are not alone. We’ve got this! Together, we can navigate this journey and embrace a brighter future. www.letsbecleartoday.com #helpisonitsway #LindaEsposito #bronchiectasis #ntmlung #pseudomonas When it comes to mask-wearing, there’s no single answer – it’s a personal decision based on individual circumstances.
I wear a mask in specific situations: *Crowded indoor spaces: This includes exercise classes with closed doors, like the Pilates class I attend, even if I’m the only one masked. *Travel: I wore a mask throughout my recent flight from California. I also wear it on trains, buses and the subway. *Hair salons: While I don’t require my stylist to wear one, I appreciate it when they do. I forgo a mask outdoors, in uncrowded spaces like big stores and large restaurants (especially at off-peak hours and with good seating options). However, if a restaurant becomes unexpectedly crowded while I’m dining, I try not to let it ruin my evening out. It’s important to remember that everyone has different risk factors. Some may be immunocompromised, have undergone surgery, have comorbidities or simply feel more cautious. This was evident at a recent support group picnic where half the attendees, even while outdoors, chose to wear masks. I respect their decision completely. Talking to your doctor and respiratory therapist helps to make informed choices about mask-wearing. Ultimately, there’s no single “right” answer. The key is to be respectful of others’ decisions and prioritize your own well-being. #Immunocompromised #CommonVariableImmunoDeficiency #Covid I have bronchiectasis (BE) and a history of Mycobacterium Avium Complex (MAC-LD) lung infections. Both were considered rare, but with increased medical professional education and the use of High Resolution CT scans, BE is being diagnosed more frequently than in the past.
When people have both bronchiectasis and a MAC infection doctors frequently say that it is a “chicken or the egg” situation. Did the bronchiectasis damage and inflammation allow the MAC to set up shop in the lungs or did the MAC infection cause the BE? Some answers to this question can be found in a person’s medical and lifestyle history. For example, having pneumonia or bronchitis might have caused the scarring in the lungs. A deeper dive might uncover genetic causes and in some cases, these underlying conditions might be treatable. Although in my case nothing is certain, I probably got the BE from a bad pulmonary infection in my mid-50s that led to inflammation and a welcoming environment for MAC. At one point, my husband and I moved out of Manhattan to upstate New York. I had a huge flower garden during the eight years we lived there and spread heaps of mulch and soil. MAC loves mulch and because it is fluffy and easily airborne, it can find its way into the lungs and for some people, cause disease. In my book, “The BE CLEAR Method to Living with Bronchiectasis” available on Amazon, https://amzn.to/333htls I mention my double-whammy diseases but focus on bronchiectasis. This was a deliberate choice as there are many people who have BE and will never get MAC or any Nontuberculous Mycobacterial (NTM) infections. At the same time, because roughly 30% of those with BE in the US will contract an NTM infection, I feel I should talk about it so people, if they so choose, can minimize their exposure. To learn more about lowering your risks, go to the Resources Page on my website letsbecleartoday.com and scroll to the very bottom where you will see an article from Dr. Joseph Falkinham. Let me know if you have any questions! PS my pulmonologist asked if she could use this photo in her slide presentations to show people what not to do with bronchiectasis and NTM lung disease!!😩😀 #Bronchiectasis #NTM #NTMLungDisease #NTMLungDiseaseSupportGroup #NTMLungDiseaseInfo #falkinham #pneumonia #bronchitis In June 2021, I began using a vibration vest to manage my bronchiectasis. A month later, I got COVID. Despite only experiencing a headache and fever, I diligently performed airway clearance 3 times a day. This period became an opportunity to get familiar with my vest and I came to view it as a powerful tool in my bronchiectasis toolkit.
Recently, I’ve heard concerns from others about the vest. Some have expectations of expelling large amounts of mucus and feel discouraged when that doesn’t happen. The high cost can also lead to frustration and a desire to return the vest. I understand this sentiment. I faced a hefty co-pay for my vest as well. Initially, I too hoped to see a dramatic increase in mucus clearance. While that wasn’t the case, I remained committed to using the vest twice daily. Six months later, I was thrilled to finally test negative for a chronic MAC infection. It’s important to note that I also made other lifestyle changes during this time. I increased my protein and calorie intake, exercise and focused on stress reduction. Therefore, I can’t solely attribute my improvement to the vest. However, I believe it played a significant role in maintaining my health. Be wary of advice suggesting the vest can replace other airway clearance methods. I’ve heard some trainers tell their clients they no longer need to use an Acapella or Aerobika and there’s no need to nebulize. This is concerning. To my knowledge, no bronchiectasis center advocates this approach. My doctor, a specialist in BE and NTM-LD, emphasizes the importance of using all three techniques. Similarly, National Jewish Health often recommends a three-pronged approach for their patients. The key takeaway is patience. I believe in the vest’s effectiveness as part of a comprehensive management plan. Stick with your treatment regimen, but don’t abandon your other tools. Think of it like protection in a terrible storm: you wouldn’t leave home without a raincoat and boots just because you got an umbrella. All three work best together. BE CLEAR with Bronchiectasis has a consulting relationship with Monaghan Medical #Hfcwo #hfcwovests #airwayclearance #sputum #phlegm I felt like a movie star years ago, walking into the Sean Parker Voice Institute in New York City. The halls were lined with signed photographs from famous actors and singers. Not being able to carry a tune made me feel out of place, but, hey, I was there to find out why I was often hoarse.
While I was sitting on the exam table, talking to the doctor, I cleared my throat. “Don’t do that!” she said. “Clearing your throat is harsh on your vocal cords and can cause inflammation. Instead take a sip of water. And, if you don’t have water available, try to suppress the urge.” I’ve done pretty well over time and I must say I clear my throat very infrequently now. Recently, reading an Instagram post by Dr. Inna Husain, an ENT, I see she also says throat clearing is a no-no. In addition to taking a sip of water she suggests if we don’t have water available to do a hard swallow. She explains that clearing our throat can traumatize our vocal cords and create a hypersensitivity and mucus. Dr. Husain suggests using .9 % saline to moisten our vocal cords. And, of course, many of us are already nebulizing for our bronchiectasis and I imagine nebbing salty saline could actually irritate our cords!!! 😱😱😱 Perhaps we could ask our medical team if it makes sense when we find ourselves clearing our throat a lot, to moisten our cords by nebulizing with .9 isotonic solution. Also, I suggest becoming more aware of when we clear our throat and to try to suppress the urge. Come up with a few ways of dealing with it, such as sucking a non-mentholated candy, taking a few puffs on Aerobika or drinking water. #throatclearing #chronicthroatclearing #mucus #phlegm #coughing #bronchiectasis #nebulizing Some with BE take showering precautions to limit exposure to steam that can harbor lung pathogens. This concern can make traveling tricky. So, let’s brainstorm about our bathing and showering options!! One solution is to find accommodations that have a bathtub. Another is to see if the accommodations have showers with a handheld fixture that allows one to target the water and minimize steam exposure. This is my go-to method in my NYC apartment, and it works great! In addition, think about the following: *Let your tap, toilet and shower run for several minutes before using water (don’t be in the room while clearing out the pipes) *Run a bathroom fan while bathing *Take short showers *Substitute sponge baths for showers *Wear a mask *Remove the showerhead as it is often the source of bacteria I recently heard from someone who brings his own showerhead! Now I call that planning a “head”:)!! Whatever our challenges, let’s be sure to not make them obstacles to enjoying ourselves. #showerprecautions #drfalkinham #maclungdisease #ntmlungdisease #bronchiectasis Some of us with bronchiectasis choose to take drinking water precautions to prevent bacterial infections. We drink water that is sterile. Options are:
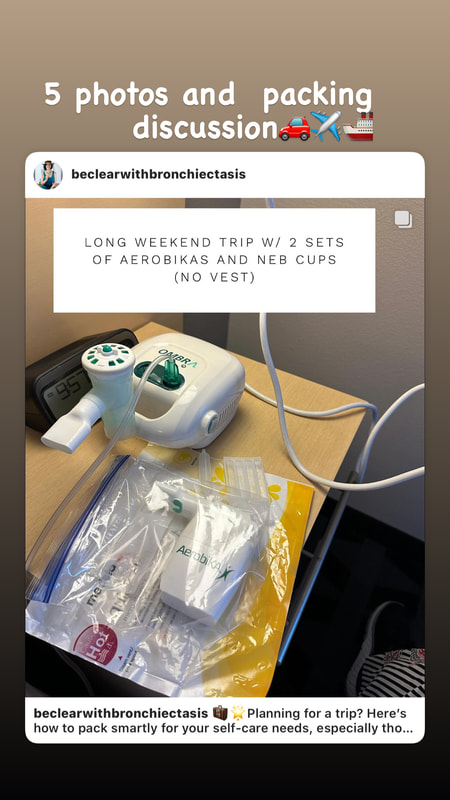
*Water from a Lifestraw pitcher or water bottle with filters (NOT a Brita filtering device). *Water from a UV water bottle or treated with a Steripen *Bottled spring water *Boiled water When traveling, some of these options might not be available or practical, but generally speaking, we can find one that works for us. I used the Steripen regularly during my trip in October to Italy and also when necessary bought bottled water. I chose not to bring my Larq UV water bottle on my trip because while sightseeing I don’t like carrying anything or wearing a backpack. But, many find it and the CrazyCap helpful. Now let’s talk about how the water we drink can cause an infection in our lungs and possibly more bronchiectasis. The answer is two-fold: by inefficient swallowing and gastric reflux. All of us micro-aspirate liquid into our lungs throughout the day. This might be from liquid “going down the wrong pipe” as can happen with swallowing issues and coughing. Gastroesophageal reflux is another way bacteria can enter the lungs. Both acid and non-acid gastric refluxate can come up from the stomach and enter the lungs. One way to help prevent reflux while traveling is to take precautions including: *Raising the head of your bed *After eating, waiting a couple of hours before lying down, doing airway clearance or exercising *Squatting down instead of bending at the waist whenever possible *Not eating trigger foods Not everyone with bronchiectasis will get a lung infection. However, there is about a 25-30% chance one will and the precautions I have laid out can reduce that probability. In Italy, I found that most restaurants were filtering their own water to cut down on plastic use. I preferred not to drink their water as I assumed it probably was not sterile. Surprisingly, quite a number of the restaurants no longer served bottled water. So, wherever you journey to, be prepared for eco-friendly restaurants by bringing your own water. #lunghealth #lunginfectionprevention #falkinham #Bronchiectasis #NTMDisease #MACDisease #Falkinham #macdisease #mucusinbackofthroat #GERD #SwallowingDifficulties #sterilewater #lifestraw Planning for a trip? Here’s how to pack smartly for your self-care needs, especially those related to airway clearance.
Know your limits: Consider how many bags you can handle comfortably. If you’re flying solo, packing light is key! Pack a carry-on specifically for your healthcare needs. Most airlines allow a medical bag with a doctor’s note. To vest or not to vest? Some people rely heavily on their airway clearance vest and will need to take it along on all trips and others have the option of traveling without it. Talk to your medical team about travel options without the vest. Vest companies often stipulate that vests be carried onboard and not checked. My Italy Packing List : 3 sets of nebulizer cups and Aerobikas 60+ vials of hypertonic saline (1 month) Pari Trek S Travel-sized nebulizer Innospire Go Battery-operated nebulizer (unreliable) Massage gun* Exercise stretch band Rescue antibiotic A nebulizer compressor tubing replacement *I chose not to bring my vest to Italy Sterilization on the go: Medela microwave steam bags Pack a small bottle of isopropyl alcohol for sanitizing Use resealable plastic bags for soaking and sterilizing equipment (Marjorie Cullinan, Yale Respiratory Therapist) Bonus tip: Consider a dual-voltage travel steamer (like the foldable “Drizzle Pot”) for easy sterilization on the go! Remember: This is just a guide! Adapt it to your specific needs and discuss your travel plans with your medical team. Best tip of all is to BOARD EARLY!! The first time I did it, I felt a little foolish, but it made all the difference. You’re not blocking the aisle as you try to get all of your stuff organized. Happy travels! Please share this blog site in your support groups, especially with people who are not on social media. I thank you in advance! #bronchiectasis #travel #bronchiectasiswarrior Struggling with lung issues? Choosing the right nebulizer setup can make a big difference! Several years ago, I upgraded to the Ombra system from Monaghan and Trudell International.
This more powerful system is what National Jewish Health (NJH), a top US lung hospital, recommends to their patients. While I haven't received care there myself, I trust their expertise. As a BE consultant, I often hear what clients treated at NJH are instructed to do. In all cases, they've been advised to use an Aerobika with an Aeroelipse XL cup and an Ombra compressor. It's important to note that patients are also advised to change the tubing regularly (every 2 months to 2 weeks depending on source) and the filter every 6 months to maintain optimal performance. While there are other good nebulizer options from Pari and Philips, each system delivers medication differently. Substituting one cup for another can affect how much medication you receive. Talk to your doctor about the best nebulizer setup for your specific needs. #bronchiectasis #lunghealth #nebulizer #nebulising #nebulizing #nebulise #aerobika #aeroeclipse #paritreks |
AuthorLinda Cooper Esposito, MPH is a health educator with bronchiectasis. She developed the BE CLEAR Method to Living with Bronchiectasis and writes with compassion and humor about this chronic lung disease. Archives
April 2024
Categories |












 RSS Feed
RSS Feed